The Complete Six-Stage Dementia Care Journey
A systematic framework for understanding what comes next and making informed decisions at every stage
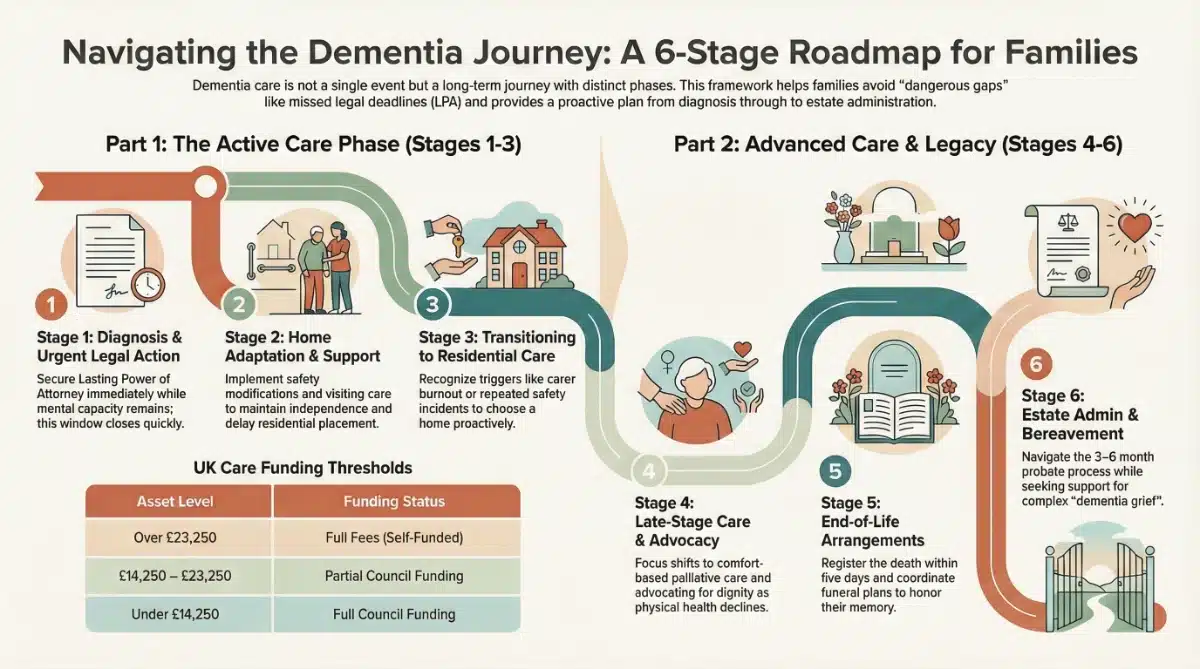
Why You Need a Framework for the Dementia Journey
When you're facing dementia—whether as a person diagnosed, a family member, or a caregiver—the journey ahead feels overwhelming and unpredictable. You're bombarded with information, advice, and opinions, but what you really need is a clear understanding of where you are now, what's coming next, and what decisions you'll need to make.
That's why we've developed this six-stage framework. It transforms an overwhelming, chaotic experience into a navigable journey with predictable phases, common challenges, and proven solutions.
This isn't about medicalizing every aspect of dementia or reducing your loved one to a checklist. It's about giving you the knowledge and tools to:
- Understand what's happening now and what's likely coming next
- Make proactive decisions rather than reactive, crisis-driven ones
- Access the right resources and support at the right time
- Plan ahead while maintaining quality of life in the present
- Feel less alone by understanding that millions of families have navigated this path before you
How to Use This Framework
The six-stage framework is not a rigid timeline. Dementia progression varies enormously between individuals—some people remain in early stages for years, while others progress more rapidly. Some stages overlap, and the boundaries between them aren't always clear.
Use this framework to:
- Identify where you are: Understanding your current stage helps you focus on relevant information and ignore what's not yet applicable
- Anticipate what's next: Knowing the likely progression helps you plan ahead without becoming overwhelmed by distant future scenarios
- Find stage-appropriate resources: Each stage has specific support needs—this framework connects you to the right tools at the right time
- Make informed decisions: Understanding typical stage progression helps you make decisions that balance current needs with future considerations
- Benchmark your experience: See how your situation compares to other families at similar stages
Not sure which stage you're in? Take our free benchmark assessment to identify your current position and get personalized recommendations.
Overview of the Six Stages
Here's what the complete dementia care journey typically looks like:
| Stage | Primary Focus | Typical Duration | Key Decisions |
|---|---|---|---|
| Stage 1 Recognition & Diagnosis | Understanding what's happening, getting diagnosis, legal planning | 3-6 months | Seeking diagnosis, arranging Power of Attorney, initial planning |
| Stage 2 Early Home Care | Managing daily life, maintaining independence, building support | 1-4 years | Home care support, safety modifications, caregiver sustainability |
| Stage 3 Increased Support Needs | Addressing inadequate home care, considering residential options | 3-6 months | Intensive home care vs. residential care, family capacity assessment |
| Stage 4 Researching Care Homes | Systematic evaluation and selection of residential care | 4-8 weeks | Choosing care home, understanding contracts, managing placement |
| Stage 5 Settling Into Care | Supporting transition, monitoring quality, redefining family role | Ongoing | Supporting adjustment, building staff relationships, care advocacy |
| Stage 6 Advanced/End-of-Life | Ensuring comfort, dignity, and peaceful death | Months to years | Advance care planning, medical interventions, end-of-life care |
Stage 1: Recognition & Diagnosis
Where you are: You've noticed changes. Memory lapses, confusion, behavioral shifts that go beyond "normal aging." You're trying to understand what's happening and whether professional help is needed.
What This Stage Involves
- Recognizing early warning signs and symptoms
- Navigating the GP appointment and referral process
- Understanding memory clinic assessments
- Receiving and processing the diagnosis
- Immediate legal and financial planning (Power of Attorney is critical)
- Beginning to educate yourself about dementia
Critical Actions in Stage 1
These must be done while your loved one still has mental capacity:
- Arrange Lasting Power of Attorney (LPA) – Both Property/Financial Affairs and Health/Welfare. This is THE most important action in Stage 1. Without it, you'll face expensive, lengthy court deputyship applications later.
- Update or create Will if not already in place
- Document current wishes about future care preferences
- Review financial situation – understand assets, income, property
- Inform DVLA of dementia diagnosis (legal requirement)
Common Mistakes to Avoid
- Delaying GP appointment hoping things will improve
- Not documenting specific incidents and symptoms before appointments
- Postponing legal planning assuming there's "plenty of time"
- Keeping diagnosis secret from family members who need to know
- Making dramatic life changes (selling home, quitting job) in panic mode
Key Resources for Stage 1
- Essential Reading:
- What is Dementia – Understanding the condition
- Types of Dementia – Alzheimer's, vascular, Lewy body, frontotemporal
- Dementia Symptoms & Early Signs – Recognizing warning signs
- Stages of Dementia – Understanding progression
- Detailed Stage 1 Guide:[Stage 1: Recognition & Diagnosis – Complete Guide]
- Support: Alzheimer's Society Dementia Connect – 0333 150 3456
Typical duration: 3-6 months from first concerns to confirmed diagnosis and initial planning completion.
Moving to Stage 2: Once diagnosis is confirmed and legal planning complete, focus shifts to managing daily life and implementing support systems.
Stage 2: Early Home Care
Where you are: Diagnosis confirmed. Your loved one is still largely independent but needs increasing support. You're learning to be a caregiver while maintaining work, family, and normal life. Home care is manageable—for now.
What This Stage Involves
- Learning dementia caregiving skills and communication strategies
- Establishing routines and home safety measures
- Managing medications and medical appointments
- Deciding whether to engage professional home care support
- Balancing independence with necessary supervision
- Caregiver self-care and preventing burnout
- Navigating benefits and funding for home care
Key Challenges in Stage 2
- Role reversal: Especially difficult for adult children caring for parents
- Work-life balance: Many Stage 2 caregivers are still employed
- Resistance to help: Person with dementia may insist they don't need support
- Driving cessation: Emotionally difficult but often necessary transition
- Managing behavioral changes: Anxiety, repetition, suspicion, aggression
- Caregiver isolation: Social activities decline as caregiving demands increase
When to Consider Professional Home Care
Signs you might benefit from home care support:
- You're exhausted and burning out
- Supervision needed during work hours
- Physical care becoming difficult
- You need respite to maintain your own health
- Companionship would benefit your loved one
Find home care support: Search our database of 10,000+ qualified home care professionals specializing in dementia care.
Key Resources for Stage 2
- Essential Reading:
- Dementia Caregiving Basics – Fundamental principles and techniques
- Daily Care for Dementia Patients: What Really Works – Practical day-to-day strategies
- Detailed Stage 2 Guide:[Stage 2: Early Home Care – Complete Guide]
- Support: Dementia UK Admiral Nurses – 0800 888 6678
Typical duration: 1-4 years, though varies significantly based on dementia type and individual progression.
Moving to Stage 3: When current home care arrangements become inadequate for safety or quality of life, and caregiver capacity is exceeded, families transition to Stage 3.
Stage 3: Increased Support Needs
Where you are: Home care is becoming overwhelming. Safety concerns are escalating. You're exhausted. The arrangements that worked in Stage 2 are no longer adequate, and you're reluctantly considering whether residential care might be necessary.
What This Stage Involves
- Recognizing when current care arrangements are failing
- Exploring intensive home care options (live-in care, increased support)
- Confronting the question: "Is it time for residential care?"
- Navigating family disagreements about care decisions
- Overcoming guilt about considering residential placement
- Managing crisis situations and hospital discharge pressure
- Understanding financial implications of different care options
Signs Current Arrangements Are Inadequate
Safety Red Flags:
- Frequent falls even with supervision
- Wandering incidents or attempts to leave home
- Fire hazards (leaving stove on despite safeguards)
- Medication errors despite management systems
- Significant weight loss from inadequate eating
Caregiver Capacity Red Flags:
- Your own health deteriorating
- Severe sleep deprivation
- Using alcohol or medication to cope
- Feeling angry or resentful toward your loved one
- Your work or family relationships in crisis
- Complete social isolation
The Residential Care Decision
Stage 3 is where most families confront the hardest question: Is residential care the right answer?
Why families choose residential care:
- Safety can no longer be ensured at home
- Quality of life improves with professional care and social engagement
- Caregiver health requires ending intensive 24/7 care
- Quality of care exceeds what family can provide
- Medical needs require professional nursing oversight
Overcoming the guilt: Almost every family experiences profound guilt about residential placement. This guilt is normal but often based on outdated assumptions about care homes and unrealistic expectations of family caregiving capacity. Choosing appropriate professional care is loving, not abandoning.
Key Resources for Stage 3
- Detailed Stage 3 Guide: Stage 3: Increased Support Needs – Complete Guide
- Financial Planning: Funding & Costs Explained
- Support: Admiral Nurses – 0800 888 6678 for help with difficult transitions
Typical duration: 3-6 months for planned transitions, though crisis situations compress this timeline dramatically.
Moving to Stage 4: Once the decision is made that residential care is appropriate (whether immediately or in near future), families move to systematic care home research and selection.
Stage 4: Researching Care Homes
Where you are: Decision made—your loved one needs residential care. Now comes the overwhelming task of choosing the right care home from hundreds of options. You want to get this right; it's one of the most important decisions you'll ever make.
What This Stage Involves
- Defining your requirements (care level, location, budget, specializations)
- Searching and filtering care home options systematically
- Understanding CQC reports and quality indicators
- Visiting and evaluating potential homes
- Asking the right questions during tours
- Comparing options objectively
- Understanding contracts and fee structures
- Making final selection with confidence
The Systematic Research Process
Step 1: Define Requirements
Clarify your non-negotiables:
- Care level needed (residential vs. nursing)
- Dementia specialization required
- Geographic boundaries
- Budget constraints
- Specific medical or behavioral support needs
Step 2: Build Shortlist
- Use DementiaCarechoices.com database to identify potential homes
- Filter by CQC ratings, location, specializations
- Review CQC inspection reports: Understanding CQC Reports guide
- Create shortlist of 5-8 homes to visit
Step 3: Visit and Evaluate
- Schedule tours of top 3-5 homes
- Use our Quality Assessment Guide during visits
- Ask comprehensive questions: Questions to Ask Care Homes
- Return visits to top 2-3 homes at different times of day
Step 4: Compare and Decide
- Use comparison tools to evaluate objectively
- Balance data with gut feeling
- Make final selection
- Review contract thoroughly before signing
Quality Indicators That Matter
Beyond CQC ratings, observe:
- Staff behavior: Respectful, patient, engaged interactions with residents
- Resident appearance: Clean, well-groomed, appropriately dressed
- Atmosphere: Calm, pleasant, homelike rather than institutional
- Activities: Meaningful engagement, not just entertainment
- Food quality: Appetizing, nutritious, residents actually eating
- Cleanliness: Clean without strong chemical smells
- Staff-to-resident ratios: Adequate staffing for quality care
Red Flags to Eliminate Homes From Consideration
- CQC rating of Inadequate or recent enforcement action
- Strong urine or fecal odors throughout home
- Residents in soiled clothing or appearing unkempt
- Staff speaking disrespectfully to or about residents
- Multiple residents distressed, calling out, agitated
- Manager refusing to show certain areas or answer basic questions
Key Resources for Stage 4
- Search Tool: Care Home Directory – Comprehensive searchable database
- Evaluation Framework: Quality Assessment Guide
- CQC Guide: Understanding CQC Reports
- Question Bank: Questions to Ask Care Homes
- Detailed Stage 4 Guide: Stage 4: Researching Care Homes – Complete Guide
Typical duration: 4-8 weeks for planned transitions; crisis situations compress this to days or weeks.
Moving to Stage 5: Once placement is confirmed and move-in date set, focus shifts to supporting the transition and settling-in process.
Stage 5: Settling Into Residential Care
Where you are: Your loved one has moved into residential care. You're experiencing relief mixed with guilt, grief, and worry. You're wondering if you made the right choice and trying to figure out what your role is now.
What This Stage Involves
- Supporting your loved one through the transition
- Managing the complex emotions of placement
- Building relationships with care home staff
- Redefining your role from caregiver to advocate
- Monitoring quality of care
- Making visits meaningful
- Reclaiming your own life after intensive caregiving
The Emotional Reality of Placement
Common family emotions are complex and often contradictory:
- Relief: Professional care provides respite after exhausting caregiving
- Guilt: About feeling relief, about "putting them in a home," about broken promises
- Grief: Loss of home-based care, symbolic acknowledgment of disease progression
- Anxiety: Are they well cared for? Did we choose correctly?
- Second-guessing: Especially if initial adjustment is difficult
All these emotions are normal. Relief doesn't mean you don't love them. Grief doesn't mean you made the wrong decision. Guilt is almost universal but usually undeserved.
The First Weeks: What to Expect
Adjustment varies widely. Some people settle quickly; others take weeks or months.
Common initial reactions:
- Confusion about where they are and why
- Repeatedly asking to go home
- Withdrawal or appearing sad
- Anger at family "for doing this"
- OR surprisingly quick adjustment (this is also normal)
Supporting adjustment:
- Visit frequently initially (daily or every other day for first 2-3 weeks)
- Stay for meals to provide familiar face
- Bring familiar items and favorite snacks
- Communicate preferences and routines to staff
- Be patient—adjustment takes time
Your New Role: From Caregiver to Advocate
Residential placement fundamentally changes your role:
What changes:
- Physical caregiving now provided by professional staff
- 24/7 responsibility transferred to care home
- Daily management (meals, medications, routines) handled by home
Your ongoing role:
- Family member: Visiting, maintaining relationship, providing love
- Advocate: Ensuring appropriate care, raising concerns
- Monitor: Observing quality, noting changes
- Partner: Working with care team, sharing information
- Connector: Maintaining links to former life and interests
Monitoring Quality of Care
Ongoing observation ensures appropriate care:
- Personal care (clean, groomed, appropriate clothing)
- Nutrition and hydration (eating adequately, weight stable)
- Emotional wellbeing (mood, engagement, staff interactions)
- Environment (clean room, personal items cared for)
- Social engagement (participating in activities, not isolated)
Red flags requiring immediate action: Unexplained injuries, signs of neglect, sudden behavioral changes, medication errors, any suspicion of abuse.
Key Resources for Stage 5
- Detailed Stage 5 Guide: Stage 5: Settling Into Residential Care – Complete Guide
- Support: Admiral Nurses – 0800 888 6678
- Safeguarding: Contact CQC (03000 616161) or local authority safeguarding for serious concerns
Duration: Stage 5 continues throughout residential care placement. Settling-in typically takes 4-12 weeks, but the advocacy and relationship-building role continues indefinitely.
Moving to Stage 6: As dementia progresses to advanced stage with significant physical decline, families transition to end-of-life care focus.
Stage 6: Advanced/End-of-Life Care
Where you are: Your loved one has reached advanced dementia. They likely cannot communicate verbally, recognize family, or perform basic self-care. You're preparing for the inevitable while ensuring their remaining time is comfortable and dignified.
What This Stage Involves
- Understanding advanced dementia and physical decline
- Making difficult medical decisions (DNACPR, treatment escalation)
- Palliative and comfort-focused care
- Recognizing signs of approaching death
- Being present at the end
- Practical matters after death
- Processing grief and bereavement
Understanding Advanced Dementia
Late-stage dementia is a terminal condition. Physical changes include:
- Bedbound or chair-bound, unable to walk
- Minimal or no verbal communication
- Difficulty swallowing, risk of aspiration
- Complete incontinence
- Frequent infections (pneumonia, UTIs)
- Significant weight loss
- Increased vulnerability to pressure sores
What they can still experience: Despite profound impairment, people in advanced dementia can still experience comfort and discomfort, emotional tone of environment, familiar presence, and sensory experiences (music, gentle touch). Hearing often remains even when all other senses have deteriorated.
Critical Medical Decisions
DNACPR (Do Not Attempt CPR)
In advanced dementia, CPR is almost never successful and causes suffering. Most families choose DNACPR to allow natural, peaceful death rather than traumatic resuscitation attempt.
Treatment Escalation Plans
Document what treatments should and shouldn't be used:
- Antibiotics for infections (when to treat vs. focus on comfort)
- Hospital admission (when appropriate vs. when to avoid)
- Artificial nutrition (PEG tubes—evidence shows these do NOT benefit people with advanced dementia)
- IV fluids and other interventions
Best Interests Decisions
Without capacity, decisions made based on:
- Previously expressed wishes
- Current quality of life
- Likelihood of treatment benefit
- Burden vs. benefit of intervention
- Family views and medical assessment
Palliative Care Focus
Care shifts from life-prolonging to comfort-focused:
- Comfort: Managing symptoms to maximize quality of remaining life
- Dignity: Respectful, person-centered care until death
- Quality over quantity: Comfort prioritized over prolonging life
- Family support: Emotional and practical support for loved ones
Most people with advanced dementia die peacefully in their care home with support from care staff, GP, district nurses, and specialist palliative care teams when needed.
Recognizing the Dying Process
Weeks to Days Before Death:
- Increased sleeping, less alert
- Decreased interest in food and drink
- Withdrawal from surroundings
- Increased physical weakness
Days to Hours Before Death:
- Changes in breathing (irregular, long pauses)
- Skin pale, mottled, cool extremities
- Restlessness or picking at bedclothes
- Congestion (rattling sounds—not uncomfortable for person)
- Decreased responsiveness
Being Present at the End
What to do during final hours:
- Be present—your loved one may be aware even without response
- Talk to them, share memories, give permission to let go
- Physical comfort—hold hands, gentle touch
- Music from their era
- Simply being there—quiet presence is enough
If you're not there when death occurs: Many people die when family is absent. This doesn't mean you failed them. Your love and years of care matter more than presence at final breath.
After Death: Practical Matters
- Registering death (within 5 days)
- Funeral arrangements
- Final care home invoice and closing accounts
- Notifying organizations (banks, pension providers, utilities)
- Estate and probate
Grief and Bereavement
Grief after long dementia illness is complex:
- Anticipatory grief: You've been grieving for years before death
- Relief and guilt: Relief their suffering ended is normal and loving—not guilt-worthy
- Complicated patterns: Delayed grief, unexpected intensity, minimal grief—all valid
Supporting yourself:
- Allow yourself to grieve without timeline
- Talk about them, share memories
- Join bereavement groups
- Professional counseling if grief is overwhelming
- Self-care and patience with yourself
Key Resources for Stage 6
- Detailed Stage 6 Guide: Stage 6: Advanced/End-of-Life Care – Complete Guide
- End-of-Life Support: Marie Curie – 0800 090 2309
- Bereavement Support: Cruse – 0808 808 1677
- Admiral Nurses: 0800 888 6678 – Support through end-of-life and bereavement
Duration: Advanced dementia can last months to several years. The dying process itself (recognizable final decline) typically unfolds over days to weeks.
Navigating Transitions Between Stages
Stage boundaries aren't always clear. Some families move smoothly through predictable progression; others experience sudden changes or crisis-driven transitions.
Planned vs. Crisis Transitions
Planned Transitions (Ideal)
- Gradual recognition of changing needs
- Time to research options and make informed decisions
- Opportunity to prepare emotionally and practically
- Proactive rather than reactive approach
Crisis Transitions (Common but Challenging)
- Sudden health event (fall, infection, hospitalization)
- Caregiver breakdown or illness
- Hospital discharge pressure
- Emergency placement decisions
How to avoid crisis transitions:
- Recognize stage changes early
- Begin preliminary research before urgent need
- Have difficult conversations before crisis forces them
- Build support network in advance
- Plan for "what if" scenarios
When Stages Overlap
Sometimes you're simultaneously in multiple stages:
- Managing Stage 2 home care while beginning Stage 3 evaluation of options
- Researching care homes (Stage 4) while still providing intensive home care (Stage 3)
- Settled into residential care (Stage 5) while also managing advanced dementia symptoms (Stage 6)
This is normal. The framework provides guidance, not rigid boundaries.
Using DementiaCarechoices.com Throughout Your Journey
We've designed our platform to support you through every stage with the right tools at the right time.
Stage-Specific Resources
- Stage 1: Educational articles about dementia types, symptoms, diagnosis process
- Stage 2: Home care professional database, caregiving guides, self-care resources
- Stage 3: Decision frameworks, financial planning tools, crisis management guides
- Stage 4: Care home directory, quality assessment tools, CQC report guidance, comparison features
- Stage 5: Settling-in support, advocacy resources, monitoring tools
- Stage 6: End-of-life planning templates, bereavement resources
Universal Tools Available at Every Stage
- Free Benchmark Assessment: Identify your current stage, compare your situation to other families, get personalized recommendations
- Care Candidates (Shortlist): Save and compare home care professionals or care homes
- Decision Tools: Frameworks for evaluating options systematically
- Community Forums: Connect with families at similar stages
- Expert Resources: Downloadable guides, checklists, templates
Our Independent Approach
Unlike commission-based referral services, DementiaCarechoices.com operates on transparent, independent principles:
- No conflicts of interest: We don't take commissions on placements
- Objective information: All providers meeting quality standards receive equal treatment
- Family-first methodology: Decision frameworks help you choose based on needs, not our financial incentives
- Professional standards: Systematic evaluation approaches developed from best practices
The Wider Context: Not Just a Medical Journey
Dementia affects every aspect of life, relationships, finances, employment, identity, and family dynamics. Understanding the six stages helps you navigate not just medical progression but the complete human experience.
Relationship Changes
- Role reversal: Adult children becoming parents to parents
- Spousal relationships: From partner to caregiver
- Family dynamics: Sibling conflicts, caregiver burden distribution
- Social connections: Isolation as social activities decline
Financial Impact
- Lost income: Reduced work hours or leaving employment for caregiving
- Care costs: Home care, residential care, specialist support
- Property implications: Selling homes to fund care
- Long-term planning: Protecting assets, inheritance considerations
Identity and Purpose
- Caregiver identity: Life consumed by caregiving role
- After placement: Loss of purpose when caregiving ends
- Post-bereavement: Rebuilding life and identity after loss
Emotional Journey
- Grief: Begins at diagnosis, continues through all stages
- Guilt: Pervasive at every decision point
- Exhaustion: Physical and emotional toll of caregiving
- Resilience: Families discover strength they didn't know they had
You Are Not Alone
Over 900,000 people in the UK are living with dementia. That means hundreds of thousands of families are navigating this journey alongside you. Every challenge you face, someone else has faced. Every decision you're struggling with, someone else has made.
This framework exists because we've learned from those who've gone before. The insights, tools, and resources available through DementiaCarechoices.com represent the collective wisdom of countless families who've navigated all six stages.
Getting Support
- Alzheimer's Society: 0333 150 3456 – Comprehensive dementia support
- Dementia UK Admiral Nurses: 0800 888 6678 – Specialist dementia nursing support
- Carers UK: 0808 808 7777 – Support for caregivers
- Age UK: 0800 678 1602 – Advice for older people and carers
- Independent Age: 0800 319 6789 – Practical and emotional support
Next Steps: Where Do You Start?
If You're Just Beginning (Stage 1)
- Seek diagnosis: Book GP appointment, document symptoms
- Read Stage 1 guide: Stage 1: Recognition & Diagnosis
- Legal planning: Arrange Lasting Power of Attorney immediately
- Educate yourself: What is Dementia, Types of Dementia
If You're Caregiving at Home (Stage 2)
- Read Stage 2 guide: Stage 2: Early Home Care
- Learn caregiving skills: Dementia Caregiving Basics, Daily Care Guide
- Consider home care support: Search home care professionals
- Access benefits: Review funding options and eligibility
If Home Care Is Becoming Overwhelming (Stage 3)
- Read Stage 3 guide: Stage 3: Increased Support Needs
- Assess objectively: Are current arrangements adequate and sustainable?
- Explore options: Intensive home care vs. residential care
- Financial planning: Funding & Costs Explained
If You're Researching Care Homes (Stage 4)
- Read Stage 4 guide: Stage 4: Researching Care Homes
- Search systematically: Care Home Directory
- Evaluate quality: Quality Assessment Guide
- Understand CQC: CQC Reports Guide
- Ask right questions: Questions to Ask
If Your Loved One Is in Residential Care (Stage 5)
- Read Stage 5 guide: Stage 5: Settling Into Residential Care
- Support adjustment: Frequent visits initially, patient presence
- Build staff relationships: Communicate, collaborate, advocate
- Monitor quality: Observe care, raise concerns appropriately
If You're Approaching End-of-Life (Stage 6)
- Read Stage 6 guide: Stage 6: Advanced/End-of-Life Care
- Advance care planning: DNACPR, treatment escalation, best interests
- Focus on comfort: Palliative approach, symptom management
- Prepare yourself: Understand dying process, access bereavement support
Not Sure Where You Are?
Take our free benchmark assessment to identify your current stage, understand how your situation compares to other families, and get personalized recommendations for next steps.
Final Thoughts: The Journey Ahead
Dementia is one of life's hardest journeys. It tests families emotionally, physically, financially, and spiritually. It changes relationships, challenges assumptions, and requires decisions you never imagined making.
But you will get through this. Millions of families have navigated this path before you, and they've survived. More than survived—they've found moments of connection, discovered unexpected strengths, created meaningful experiences despite the disease, and ultimately ensured their loved ones received dignified, compassionate care.
This six-stage framework is your roadmap. It won't make the journey easy, but it will make it navigable. It transforms overwhelming uncertainty into a series of manageable stages with predictable challenges and proven solutions.
At each stage, you'll make the best decisions you can with the information and resources available to you. That's all anyone can do. Give yourself permission to:
- Not be perfect
- Make mistakes and learn from them
- Ask for help when you need it
- Prioritize your own wellbeing alongside theirs
- Feel whatever emotions arise without judgment
- Make difficult decisions that prioritize quality of life
You're doing something profoundly difficult and profoundly loving. That deserves recognition.
DementiaCarechoices.com exists to support you through every stage of this journey. We're here with the tools, information, and community you need, exactly when you need them.
You've got this. And we've got you.
Ready to Take the Next Step?
Identify where you are and get personalized guidance:
Take Our Free Benchmark Assessment →
Explore stage-specific resources:
- Stage 1: Recognition & Diagnosis
- Stage 2: Early Home Care
- Stage 3: Increased Support Needs
- Stage 4: Researching Care Homes
- Stage 5: Settling Into Residential Care
- Stage 6: Advanced/End-of-Life Care
Search for care support:
- Search Care Homes (Stage 4)
Need help now?
- Alzheimer's Society: 0333 150 3456
- Dementia UK Admiral Nurses: 0800 888 6678
- Carers UK: 0808 808 7777
Last updated: February 2026
About DementiaCarechoices.com: We're an independent dementia care directory providing systematic decision frameworks, transparent quality insights, and professional methodology—without conflicts of interest. Our goal is to help families make informed decisions at every stage of the dementia care journey.
